Understanding Coeliac Disease: Causes, Symptoms, and Treatment
Coeliac disease is a serious autoimmune condition in which the body’s immune system reacts abnormally to gluten, a protein found in wheat, barley, and rye. This reaction damages the lining of the small intestine, leading to poor absorption of essential nutrients. Often underdiagnosed, this gluten-related disorder can affect people of all ages and may cause a wide range of digestive and non-digestive symptoms if left untreated.
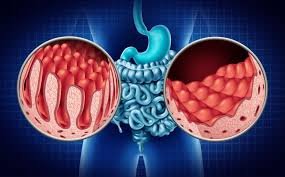
What is Coeliac Disease?
Coeliac disease is an autoimmune condition in which the immune system reacts abnormally to gluten, a protein found in wheat, barley, and rye. This immune response damages the lining of the small intestine, leading to poor absorption of essential nutrients. It can affect people of all ages and is often underdiagnosed because symptoms vary widely from person to person.
Causes of This Condition
This disorder develops when genetic susceptibility combines with an abnormal immune response to gluten. Understanding the causes helps identify people who may be at higher risk.
1. Genetic Factors
The condition often runs in families. Individuals carrying HLA-DQ2 or HLA-DQ8 genes are more likely to develop it. Having a first-degree relative with the disorder increases risk.
2. Immune System Malfunction
When gluten is consumed, the immune system mistakenly treats it as harmful. This reaction damages the intestinal villi, reducing the body’s ability to absorb nutrients properly.
3. Environmental Triggers
Certain external factors may trigger symptoms in genetically predisposed individuals, including:
Viral or bacterial infections
Changes in gut microbiota
Severe physical or emotional stress
Early gluten exposure in infancy (rare cases)
4. Other Risk Factors
People with Type 1 diabetes, autoimmune thyroid disorders, or Down syndrome have a higher likelihood of developing this condition.
Note: Risk factors increase susceptibility but do not guarantee disease development.
Symptoms You Should Not Ignore
Symptoms vary and may affect the digestive system as well as other parts of the body. Common signs include:
Persistent diarrhea or constipation
Bloating and abdominal discomfort
Unexplained weight loss
Chronic fatigue
Iron-deficiency anemia
Itchy skin rashes
Bone or joint pain
Delayed growth in children
Some individuals may have minimal digestive symptoms yet still experience vitamin and mineral deficiencies.
How Is It Diagnosed?
Diagnosis usually involves a combination of tests:
Blood tests to detect antibodies such as anti-tTG or EMA
Endoscopy with biopsy to assess damage to the intestinal lining
Genetic testing to check for HLA-DQ2 or HLA-DQ8 genes
⚠️ Important: Do not eliminate gluten from your diet before testing, as it may lead to inaccurate results.
Treatment and Management Options
Although there is no permanent cure, the condition can be effectively controlled with proper care.
Strict gluten-free diet: Complete avoidance of wheat, barley, and rye
Nutritional supplements: To correct vitamin and mineral deficiencies
Regular follow-ups: Monitoring recovery and nutritional status
With consistent dietary management, most individuals experience significant symptom relief and intestinal healing.
Living a Healthy Life
Managing this condition requires lifestyle awareness in addition to diet changes:
Read ingredient labels carefully
Prevent cross-contamination in kitchens
Inform family and friends about dietary needs
Join support groups for guidance and encouragement
Conclusion
This autoimmune digestive disorder can have serious health consequences if left untreated. However, early diagnosis and long-term dietary management allow most people to live healthy, active lives. Anyone experiencing persistent digestive or unexplained symptoms should seek medical evaluation.
FAQs on Coeliac Disease
Q1: Can this condition start in adulthood?
Yes, symptoms may appear at any age, even if gluten was previously tolerated.
Q2: Is a gluten-free diet suitable for everyone?
It is essential for diagnosed individuals but not recommended for those without medical need.
Q3: How long does intestinal healing take?
Improvement often begins within months, while full recovery may take up to two years.
