Liver Cancer: Causes, Symptoms, Stages & Treatment Options
Introduction
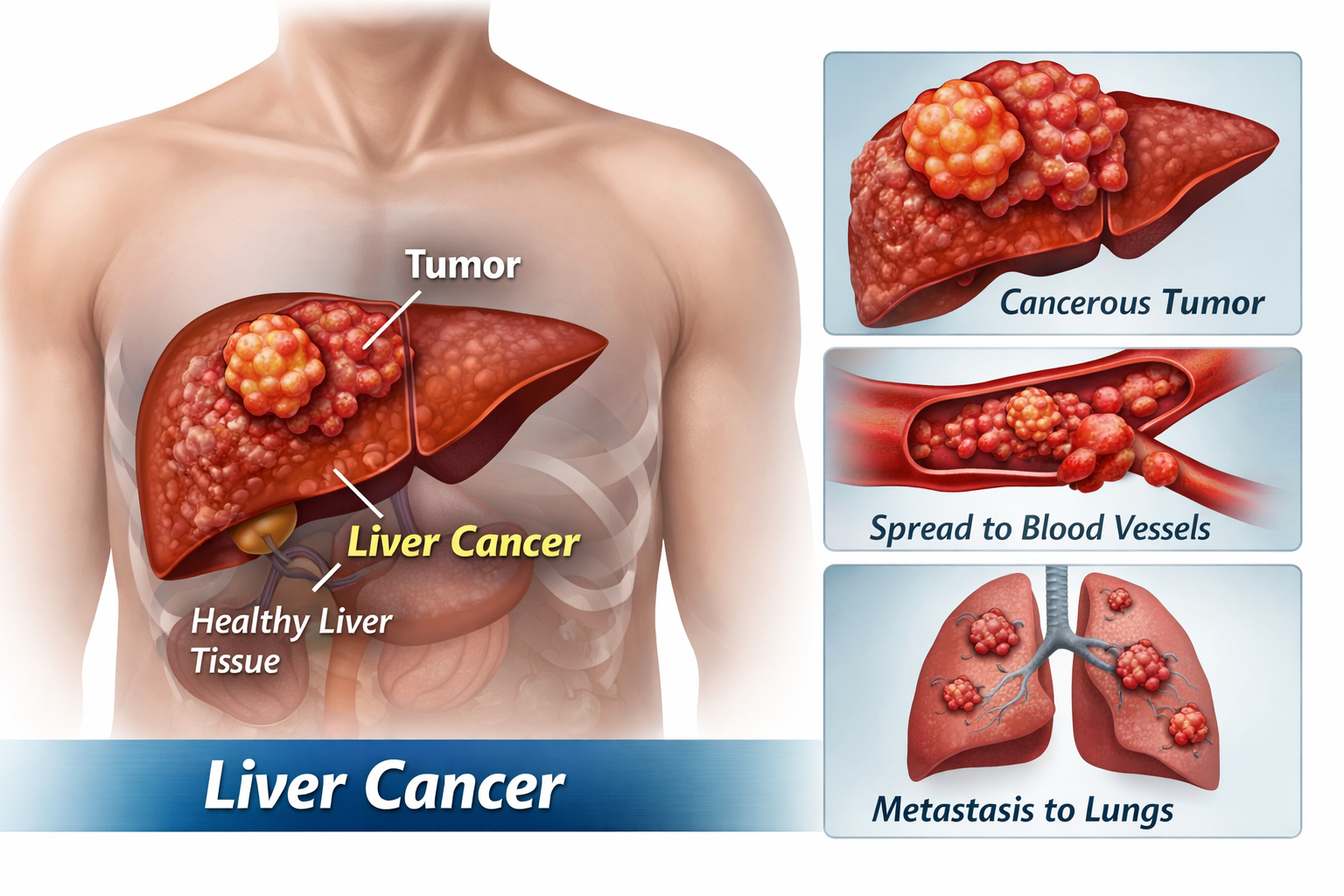
Liver cancer is a serious condition that develops in the cells of the liver. This vital organ helps with digestion, detoxification, and nutrient storage. When abnormal cells grow uncontrollably, they form a liver tumor that can interfere with normal body functions. Early detection significantly improves treatment outcomes.
Types of Liver Tumors
1. Hepatocellular Carcinoma (HCC)
The most common type of primary hepatic cancer, beginning in hepatocytes (main liver cells).
Intrahepatic Cholangiocarcinoma
A rare cancer that starts in the bile ducts within the liver.
3. Hepatoblastoma
A rare liver malignancy usually seen in young children.
Causes and Risk Factors
Several factors increase the risk of developing cancer of the liver:
Chronic infection with Hepatitis B
Chronic infection with Hepatitis C
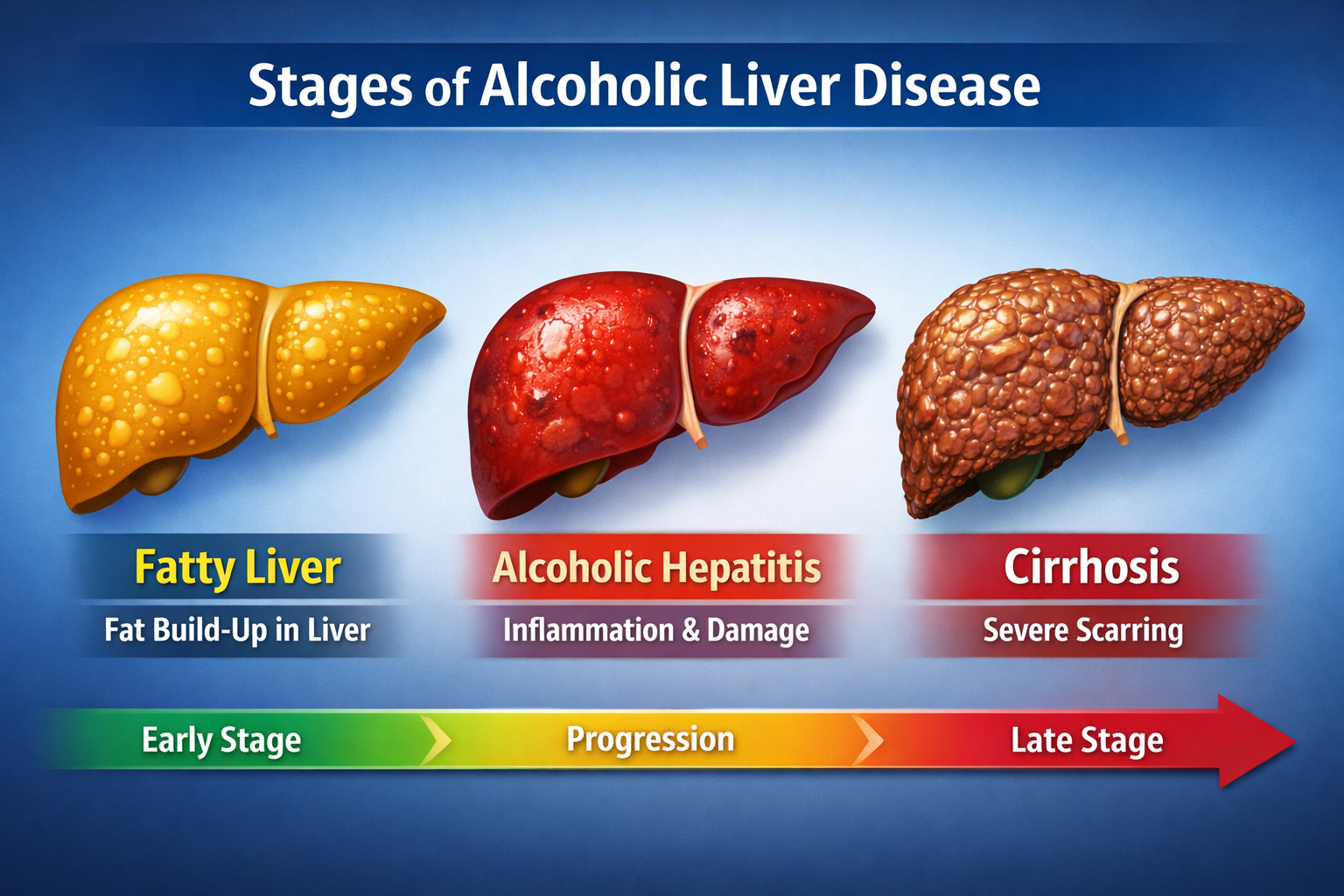
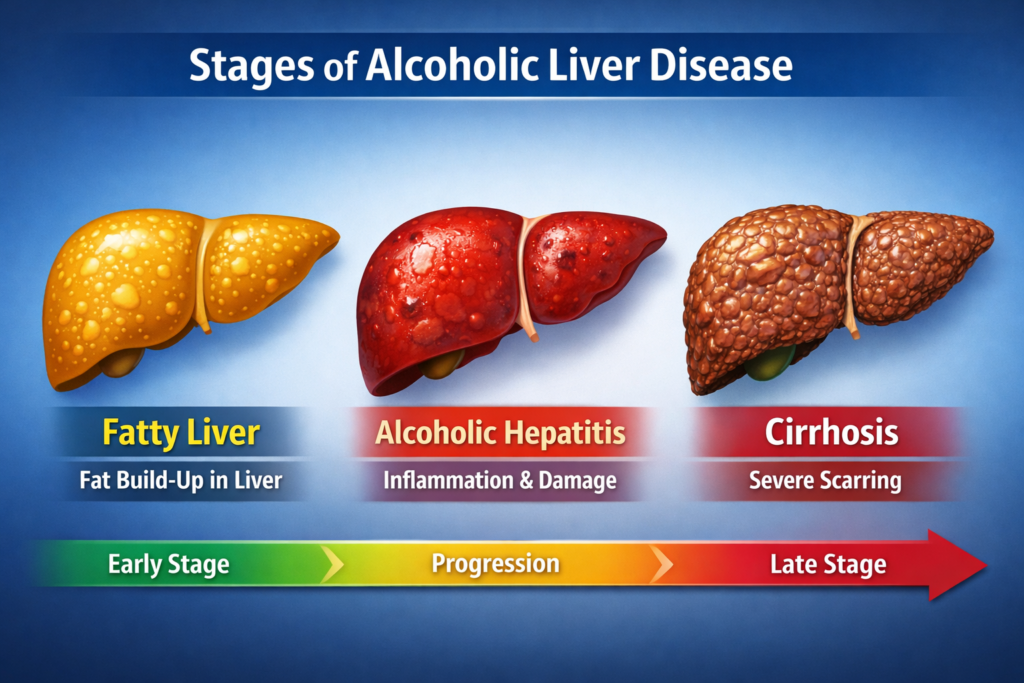
Cirrhosis (long-term liver damage)
Heavy alcohol consumption
Non-alcoholic fatty liver disease
Obesity and diabetes
Exposure to aflatoxins
Long-term inflammation and liver damage are major contributors.
Symptoms
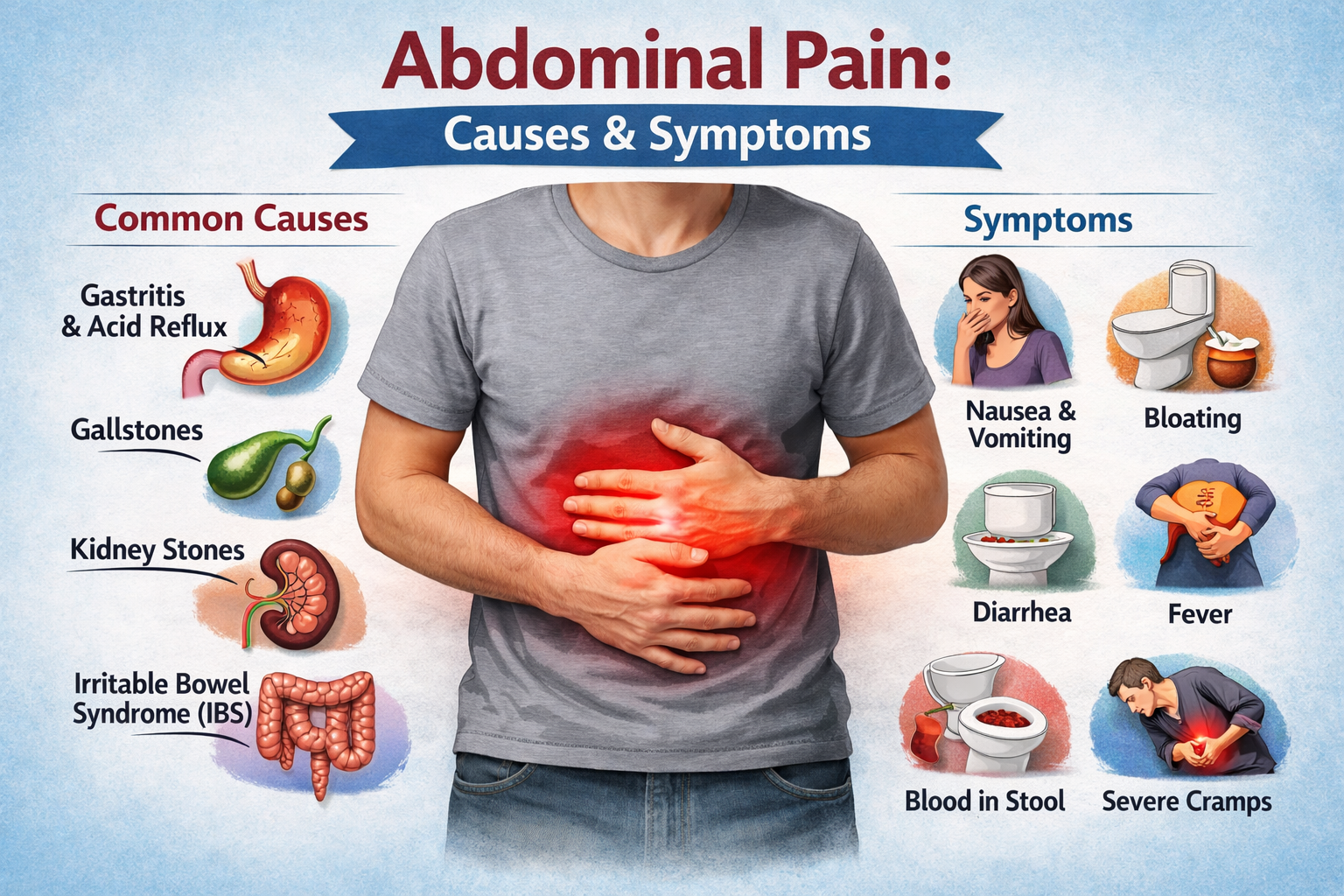
Early stages may not show noticeable signs. As the condition progresses, symptoms may include:
Unexplained weight loss
Loss of appetite
Upper abdominal pain
Jaundice (yellowing of skin and eyes)
Abdominal swelling
Fatigue
Persistent symptoms should always be medically evaluated.
Diagnosis
Doctors may use:
Blood tests (AFP tumor marker)
Ultrasound
CT scan
MRI
Liver biopsy
Health organizations such as the World Health Organization and American Cancer Society provide detailed clinical guidance on diagnosis and management
Staging
The disease is categorized into stages I–IV depending on tumor size, spread to blood vessels, and metastasis to other organs.
Staging helps determine the most effective treatment approach.
Treatment Options
Treatment depends on tumor stage, liver function, and overall health.
Surgical removal (partial hepatectomy)
Liver transplant
Ablation therapy
Chemotherapy
Radiation therapy
Targeted therapy and immunotherapy
Advanced treatment methods have significantly improved survival rates in recent years.
Prevention
While not all cases are preventable, risk can be reduced by:
Vaccination against Hepatitis B
Limiting alcohol intake
Maintaining healthy weight
Managing diabetes
Regular screening for high-risk individuals
Conclusion
Liver cancer remains one of the leading causes of cancer-related deaths worldwide. However, early screening, lifestyle modifications, and modern treatment options offer hope. Raising awareness about symptoms and risk factors plays a critical role in improving survival and quality of life.